
I had a really smooth sailing pregnancy, apart from the extreme fatigue in the first trimester, I felt great and enjoyed being pregnant. I was one of “those” who loved it! I never had any nausea or morning sickness, no blood sugar issues, etc. The biggest wrench was COVID, yeah, I gave birth during a pandemic (#laborinthetimeofcorona). You can read more about my pregnancy and type 1 diabetes in this post.
Before I get to my birth story, I wanted to share more about my pump/CGM. I used a Medtronic 670G pump and a Dexcom G6 sensor. Right before I went in for induction, I inserted a new sensor and pump site so I knew they would be working perfectly for the first few days as a new mama. I placed my CGM and pump site on my arms, each on different sides. There were LOTS of blood pressure checks, but my pump site didn’t really hurt or cause any issues. Anyway…
Here’s my birth story:
I was induced on Mother’s Day, May 10th, 2020, in the evening around 9pm. I was 1cm dilated and 50% effaced, so we started induction with a foley bulb and cytotec (oral). The foley bulb insertion really wasn’t painful for me, similar to a cervical check. It didn’t take long to start having regular contractions, but they weren’t painful and I could barely feel them. My body was really working hard though, as I had to reduce my basal rate by 25%. I couldn’t sleep much that night as I was being given cytotec every 2 hours, which meant constant interruptions, plus I was excited and nervous about what was yet to come – meeting my baby! By 5:00am I was contracting regularly enough that we stopped cytotec. I also had to reduce my basal by 50% due to my body starting to work much harder. The foley bulb can only be placed for 12 hours, so at 9am it was removed. I was 3cm and 50% effaced. At this time, I also had a membrane sweep to help me progress a bit more naturally. Honestly, the worst part was the lack of sleep overnight.
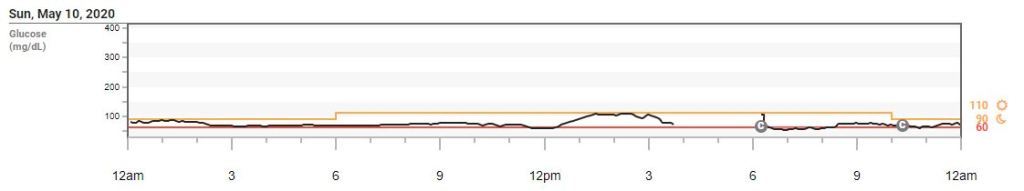
I made the decision to reduce my basal a few times, as mentioned above, when I noticed that I was constantly trending lower. It was a very gradual trend down, but it was enough to need to reduce my basal rate. I wanted to stay between 70-100 during labor and delivery; that was my goal.
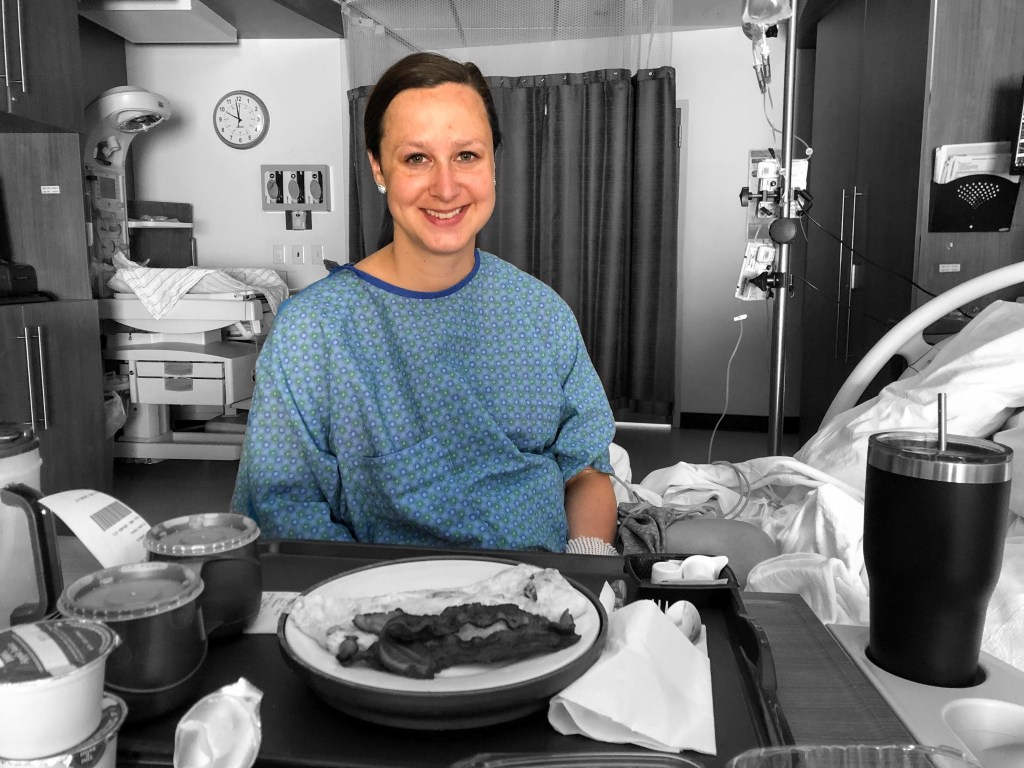
We ordered breakfast and I got an omelette. My biggest tip would be to eat something that is lower in carbs to reduce blood sugar variability, but full of protein to help with hunger. Protein also helps with expending energy later on. Again, a low carb high protein meal is perfect for keeping blood sugars stable and feeling satiated!
Around 9:45am Pitocin was started and every hour it was increased. Let me tell you, Pitocin contractions are no joke! It was almost immediate that I could tell things were going to move quickly. Thankfully, I was able to be hooked up to portable machines, so I could walk the halls and my room. Two things were incredibly annoying that prevented me from walking and moving around as much as I wanted. First, the machines weren’t charged enough, so I had to wait before walking. Second, when they were finally charged, the hospital Endocrinologist came into the room to go over my control and plan for deliver and postpartum.
I absolutely HATED the hospital endo. I self-managed my diabetes the entire pregnancy, didn’t have an A1C higher than 5%, yet the endo literally had the audacity to say he was concerned about my control. I laughed out loud until I realized he was serious. I asked him why he would be concerned about normal blood sugars. SERIOUSLY?! His response is that low blood sugars are dangerous. Again, I gave him my Dexcom data and asked him to tell me where that’s been happening. Needless to say, he had no response and we ended the conversation. He gave me a postpartum plan and I regret following it to this day. It was the most negative part of my birth experience and I should have self-managed like I did the entire time prior, but I trusted him. I should have known better. More on that later…
By 11:30am I was having extremely painful contractions and could no longer concentrate or walk down the halls (with a mask on, COVID). I kept doubting that I could do it without pain meds, which was my goal. I’m pretty sure I yelled multiple times that there was no way I could do it; the pain was nearly unbearable. I wouldn’t have been able to do it without my husband. He was the most incredible birth partner, squeezing my hips and talking me through contractions. P.S. he read “The Birth Partner” by Penny Simkin and I could definitely tell! He was also in charge of checking my Dexcom throughout the day and this was crucial when it came to the pushing stage.
Shortly after 1pm I felt like I was going to poop with each contraction. Based on everything I read during pregnancy, I knew this meant that I was super close to pushing! There was some serious pressure going on and it turns out it was just Anja making her way down lower and lower. At that point, the nurses took me very seriously. I was checked and I was 10cm and ready to push. I also suspended my insulin pump at this time because pushing is literally like running a marathon. I honestly don’t remember much of the 2 hour pushing phase, except that it honestly felt like a relief to the contractions. Seriously. It was so much better than working through them. Again, my husband was checking my Dexcom every 15-30 minutes to make sure I was in range. The nurses were also checking my blood sugar via finger pokes every 30 minutes, but I literally have zero recollection of it happening. I was in another world. So if you’re reading this, make sure you have someone who will keep an eye on things for you; chances are, you won’t be in the right state of mind to do it yourself.
Thankfully, with the help of my husband and nurses, when I gave birth, my blood sugar was around 110 mg/dl. This was higher than I would have liked to be, but in all honesty, it was just fine. Anja did not have any low blood sugars after birth, although, she did 26 hours later. She was fine, but they did treat it with a bit of glucose. She didn’t have any issues related to blood sugar that kept us separated or caused any concerns. That is why it is absolutely imperative that blood sugars are controlled during labor and delivery. Babies can overcompensate their own insulin production based on mom’s blood sugar, resulting in lows for them. This usually happens within the first hours after birth.

At 3:44pm Anja made her entrance to the world, all 6lb 2oz and 19 inches of her + loads of dark hair! Mothers with type 1 diabetes are not automatically destined to have big babies! With tight blood sugar control, this can be prevented.
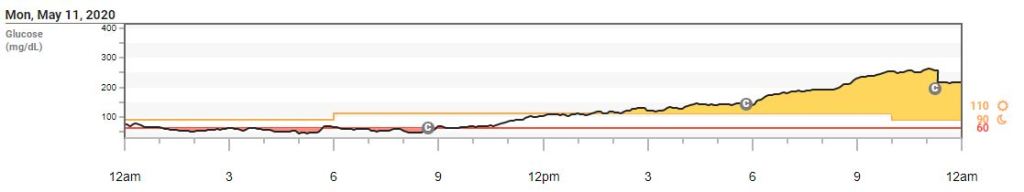
Here’s the kicker. I had the toughest time with my blood sugar post-delivery because of the hospital endo’s suggestions. He suggested that I keep my pump off until I reached 200 mg/dl. I don’t know why I listened. I’m literally still upset about it. Thinking back, I followed his advice because I had heard that once the placenta is delivered, insulin needs stop for a while, then pick up at a much lower rate. So I assumed this would happen to me. Well, I ended up letting it climb to 180 mg/dl before I intervened and started my postpartum basal rate. By that time, it was too late. I was dealing with resistance and had a hard time getting back down in range. I hadn’t been that high for over three years (YES, I did not have a blood sugar higher than 180 mg/dl in 3 years). As you can see below, I wasn’t back below 100 mg/dl until 24 hours after birth.

I have a lot of regrets over this. I had brain fog and fatigue from high blood sugars, and I just wasn’t able to be myself. Again, I hadn’t been that high in YEARS, so on top of feeling terrible from giving birth, I was dealing with out of control blood sugars.
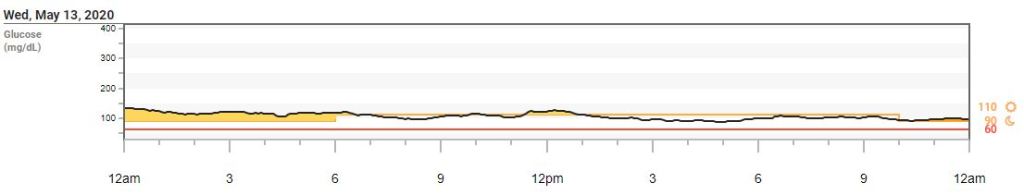
Thankfully, once I got my blood sugars back down, they were easy to manage again. My basal rate was a fraction of what it was pre-pregnancy (and still is 5.5m PP, breastfeeding).

Basal rates:
Basal 1: pre-pregnancy
Basal 2: week 16 change
Basal 3: week 23 change
Basal 4: week 30/32 change
Basal 5: after delivery & PP while breastfeeding

I was also prepared to experience low blood sugars from breastfeeding. Thankfully that never happened, but many women do experience this.
I managed labor with no pain medication. I’m still not sure how I did it, but it was one of the most empowering and incredible experiences of my life.
And now we have the most beautiful little girl, Anja. We are over the moon in love with her.

Anja 💓


1 Comment